Craig Williamson
MGH/BWH Neurology Resident
It is certainly with reluctance that I leave Uganda and return to the US. Working here has been an educational and humbling experience that challenged me to think about how to manage common and uncommon neurological conditions without the resources available at MGH or the Brigham. On my final day, I prepared a talk for the post-graduates on the clinical evaluation and differential diagnosis of spinal cord disorders. Just before the talk, I was called to the ED to examine a 22 year-old woman who has had one month of progressive lower extremity weakness, progressing to total inability to walk. She had been seen in the ED four days prior and had been sent out to get plain X-rays of her lumbosacral spine, which not surprisingly appeared normal. On examination, she had flaccid weakness of the lower extremities with extremely brisk reflexes, sustained clonus in the ankles and upgoing toes - without any upper extremity symptoms her problems easily localize to the thoracic spinal cord. For all of my recently acquired knowledge about the many causes of myelopathy in tropical settings, it wasn't at all clear to me how to proceed with her evaluation and treatment. At MGH, she would be admitted, have an MRI of at least her thoracic spine, probably also of her cervical spine and brain, then would undergo a lumbar puncture that would be sent for a dizzying array of laboratory tests for infectious and inflammatory causes of myelopathy, in addition to other tests for various metabolic and nutritional causes. Depending on our determination of the etiology, she would most likely be treated with a course of high-dose steroids. It was informative to talk through the case with the post-graduates and get their recommendations on how they would manage the patient without MRI and most laboratory tests. Essentially, they would probably test her for HIV and then treat her for things they can treat - most likely TB. My own uncertainty with the case illustrates how difficult it is to come in to an unfamiliar setting for a short period of time and make constructive management recommendations.
Fortunately, another of my colleagues from the MGH/BWH neurology residency will be visiting Mbarara in just a few weeks and can build on some of the things I learned. In addition to spending more time working with the very eager medical students, we can hopefully develop some clinical protocols to assist with management of common neurological issues. In particular, there appears to be a tremendous need for improved prevention and management of traumatic brain injuries - one of the most common reasons for ICU admissions - though it isn't at all clear how best to do this with less access to CT scanning and laboratory testing. This is just one of many potential areas of academic inquiry that would be extremely rewarding to pursue.
Here, one of the medicine post-graduates waxes eloquently to the third-year students at the beside about the subtypes of Guillain-Barre syndrome and the side-effects of treatment with IVIG, which isn't available at MRRH.
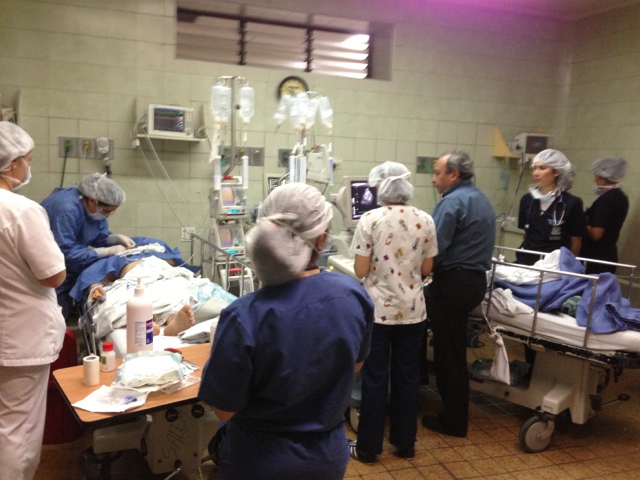
An 8 bed ICU was recently opened in MRRH's new building. The use of motorcycles as the primary means of transportation in Mbarara - typically without helmets for the drivers or passengers - leads to an extremely high volume of TBI requiring neurosurgical intervention.
Some of the talented post-graduates waiting for me to begin my final talk.
Looking silly for the sake of education as I attempt to act out features of an MCA stroke.
MGH/BWH Neurology Resident
It is certainly with reluctance that I leave Uganda and return to the US. Working here has been an educational and humbling experience that challenged me to think about how to manage common and uncommon neurological conditions without the resources available at MGH or the Brigham. On my final day, I prepared a talk for the post-graduates on the clinical evaluation and differential diagnosis of spinal cord disorders. Just before the talk, I was called to the ED to examine a 22 year-old woman who has had one month of progressive lower extremity weakness, progressing to total inability to walk. She had been seen in the ED four days prior and had been sent out to get plain X-rays of her lumbosacral spine, which not surprisingly appeared normal. On examination, she had flaccid weakness of the lower extremities with extremely brisk reflexes, sustained clonus in the ankles and upgoing toes - without any upper extremity symptoms her problems easily localize to the thoracic spinal cord. For all of my recently acquired knowledge about the many causes of myelopathy in tropical settings, it wasn't at all clear to me how to proceed with her evaluation and treatment. At MGH, she would be admitted, have an MRI of at least her thoracic spine, probably also of her cervical spine and brain, then would undergo a lumbar puncture that would be sent for a dizzying array of laboratory tests for infectious and inflammatory causes of myelopathy, in addition to other tests for various metabolic and nutritional causes. Depending on our determination of the etiology, she would most likely be treated with a course of high-dose steroids. It was informative to talk through the case with the post-graduates and get their recommendations on how they would manage the patient without MRI and most laboratory tests. Essentially, they would probably test her for HIV and then treat her for things they can treat - most likely TB. My own uncertainty with the case illustrates how difficult it is to come in to an unfamiliar setting for a short period of time and make constructive management recommendations.
Fortunately, another of my colleagues from the MGH/BWH neurology residency will be visiting Mbarara in just a few weeks and can build on some of the things I learned. In addition to spending more time working with the very eager medical students, we can hopefully develop some clinical protocols to assist with management of common neurological issues. In particular, there appears to be a tremendous need for improved prevention and management of traumatic brain injuries - one of the most common reasons for ICU admissions - though it isn't at all clear how best to do this with less access to CT scanning and laboratory testing. This is just one of many potential areas of academic inquiry that would be extremely rewarding to pursue.
Here, one of the medicine post-graduates waxes eloquently to the third-year students at the beside about the subtypes of Guillain-Barre syndrome and the side-effects of treatment with IVIG, which isn't available at MRRH.
An 8 bed ICU was recently opened in MRRH's new building. The use of motorcycles as the primary means of transportation in Mbarara - typically without helmets for the drivers or passengers - leads to an extremely high volume of TBI requiring neurosurgical intervention.
Some of the talented post-graduates waiting for me to begin my final talk.
Looking silly for the sake of education as I attempt to act out features of an MCA stroke.